News Team member Caroline Hansen reports that hospital closures across the United States threaten equitable healthcare access for rural populations and demand solutions.
Overturning the Right to Legal Abortion Poses a Danger to the Future of Medicine in the US
Bans and restrictions created in the year since the Dobbs decision undermine not just medical care, but education and training too
By Rebecca Sugerman
On June 24, 2022, the U.S. Supreme Court overturned Roe. v Wade, taking away the constitutional right to abortion. Roe was overruled with Dobbs v. Women’s Health Organization, a case that was raised because the Women’s Health Organization challenged Mississippi’s Gestational Age Act, which did not allow abortions after 15 weeks of pregnancy.
Now, abortion laws and reproductive policies are dictated by individual states. Since this decision, thirteen states have fully banned abortions, with nine of those states making no exception for incest or rape. Other states have imposed abortion bans after 6, 15, 18, and 20 weeks of pregnancy. These policies require an abortion either before or right after the first trimester of pregnancy.
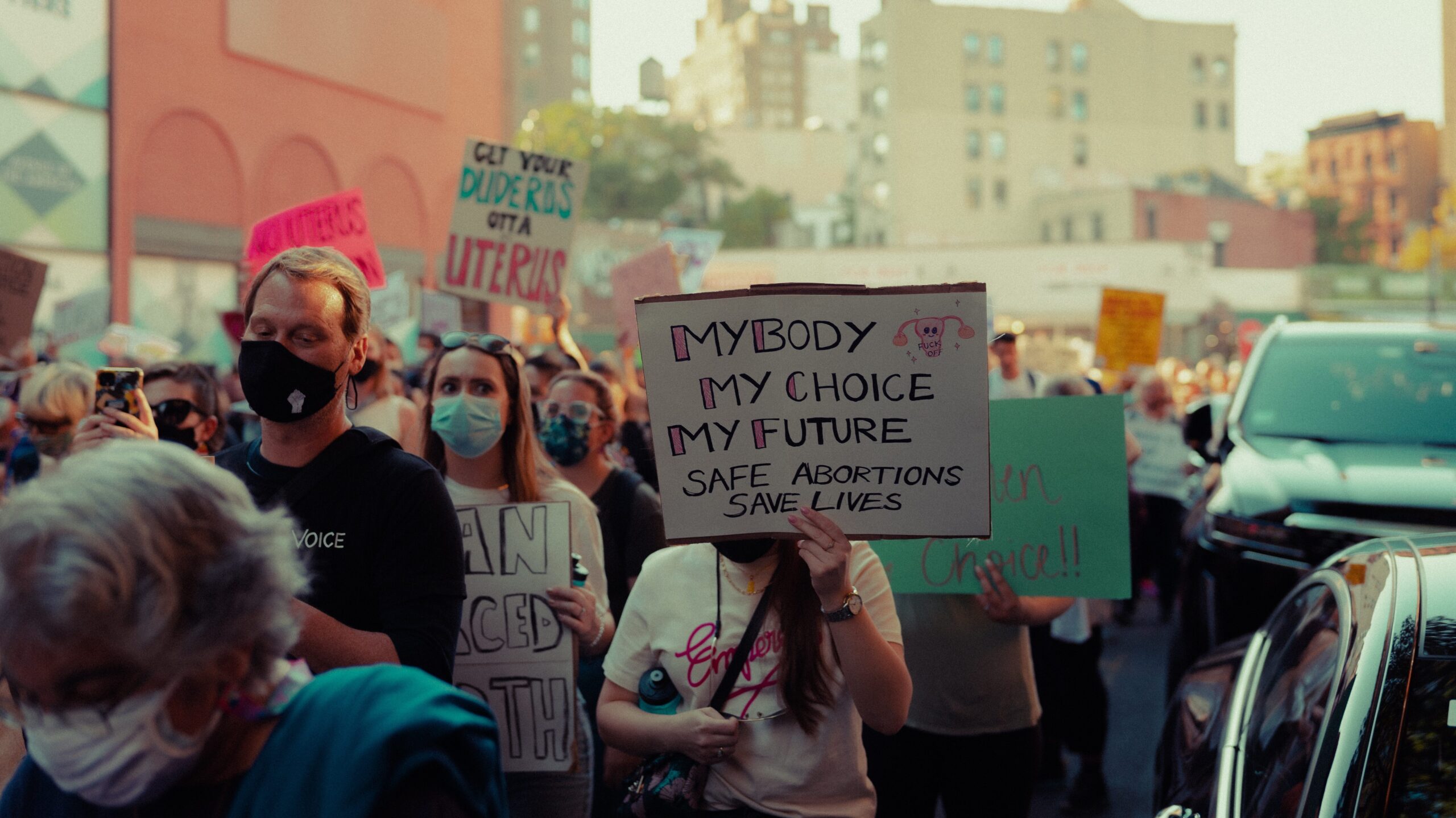
Not only do these abortion bans affect pregnant individuals’ health and safety, but they impact medical students and their access to adequate reproductive training. Students, residents, and fellows in states where there are strict abortion laws are at a disadvantage due to the now limited educational resources. As a result of overturning Roe, many teaching clinics were forced to close and numerous medical school programs cannot allocate sufficient resources for training.
Overturning Roe will have immense and lasting effects. All students completing their medical training, as well as physicians and administrators in this field, will feel this greatly, and they are concerned about the future of reproductive care.
Abortion was not legalized nationally until Roe v. Wade was decided in 1973. In just the first year, the maternal mortality rate decreased by 50 percent. Likewise, since Roe was overturned, maternal death rates were found to be 62 percent higher in abortion-restricted states. Roe had a major impact on the safety and mortality rates of women in the United States, and without this protection or proper training, women’s health is at risk.
“These restrictive laws are interfering with us providing safe, effective, ethical health care for our patients,” said Dr. Carrie Cwiak, MD, MPH, an OB-GYN and professor and director of the Division of Family Planning at Emory School of Medicine. “We can’t do it because of the law, and that causes significant distress.”
Medical students will also be limited in their training and ability to provide future abortion care. Under this ruling, almost 71 percent of medical students will experience restricted abortion training due to state laws, with only around 29 percent of medical students being educated and trained in states that protect abortion rights.
Dr. Alyssa Stephenson-Famy, MD, Associate Professor in the division of Maternal Fetal Medicine and Associate Residency Program Director at the University of Washington, has experienced this first-hand. The University of Washington has campuses across five states, and Stephenson-Famy had to restructure lesson plans so they could be taught at one of their campuses in Idaho. In Idaho, abortion is only legal in cases of sexual assault or rape, so she put a sexual assault case in the curriculum in order to teach about abortions.

“I wouldn’t normally have done that because that’s not the point of teaching the material,” Stephenson-Famy said. “But we wanted to make it a realistic enough scenario that it would be able to be taught legally, in every state.”
While Stephenson-Famy is trying to keep abortion education in the University of Washington’s curriculum, she is concerned about how other schools and their students will approach pregnancy complications and other aspects of women’s health. “We’ve been really worried about coverage of ectopic pregnancy and molar pregnancy and miscarriages,” she said. “I think that’s one of the most concerning things because some of the medications used for medication abortion are also used for those conditions.” She is concerned that students in restricted states will not learn how to manage these types of pregnancies and miscarriages based on the laws of the state their school is in.
The surgical procedure used for early pregnancy loss is essentially the same as the procedure performed for an abortion. While this provides a small benefit to students, exposing them to the procedure even if abortions are not being discussed, it also means that this might be the only exposure students receive. With abortion education in medical school being variable to begin with, this poses a huge issue.
“Not only are our learners going to have less opportunity to learn about abortion care, but they’re going to have less opportunity to learn about early pregnancy loss care, like miscarriage,” Cwiak said. “So it really does still impact the counseling experience that people get.” She recognizes that this poses a challenge when counseling patients, as well as stunts the student’s learning experience.
Stephenson-Famy is also worried about the future of reproductive care, especially in terms of having adequately trained physicians. “This is a really life-saving procedure for people who are having emergencies, people who are hemorrhaging, or people who are septic,” she said. “We need to have a generation of providers who feel comfortable with the procedure for eternity. We can’t have it die with this generation. We need to make sure that people are well trained forever because no one else can do this procedure.”
OB-GYNs and professors are not the only ones feeling the effects of the ruling and expressing concern. Ariana Traub and Nell Mermin-Bunnell, students at Emory University School of Medicine, conducted a survey to evaluate its impacts on third and fourth-year medical students. While the results of the survey are not published yet, they shared that location was clearly a big factor affecting where students were applying for jobs and planning to continue their medical career, regardless of specialty.
Students and residents are finding it more important to consider the state they are studying in because the legislature will affect their education and future practice as a doctor. Cwiak echoed this observation, stating that Emory’s Complex Family Planning department saw a 50 percent decrease in their fellowship application this past year.
If medical students are hesitant to go to school and practice in restricted states, then patients in those states will not have access to adequate pregnancy-related healthcare. Georgia already has an obstetrician shortage, with many counties not having an obstetrician. “So, if you’re making it even harder to recruit an OB-GYN to our state, that is going to impact healthcare access even more,” Cwiak said. “We are already the second worst state for maternal mortality. We’re just going to see that rise.”

Traub and Mermin-Bunnell feel these limitations. Both students were excited to study in Atlanta and work at Grady Hospital, but they did not realize how much state legislature would inhibit their ability to have the impact they were hoping for. “I think that I am not able to be an advocate for my patients in the way that I would want to,” said Mermin-Bunnell. “That’s our job, as future physicians, to deal with challenging ethical questions. I feel somewhat limited in my capacity to really dive deep into those questions because of the legal political landscape.”
Overturning Roe goes beyond outlawing abortion. The decision has country-wide implications regarding sufficient access to healthcare. “I don’t think that anybody really considered that people are trained in one state, and they are not going to practice there forever,” Stephenson-Famy said. “Everyone needs to be trained in the same stuff; you can’t just have state-specific types of OB-GYNs. That doesn’t make sense and it’s not how medicine works. We can’t have state-specific variation like this because it creates big holes in the number of providers.”
The future of accessible and equal reproductive care is at stake, and overturning Roe has already created issues and stress across the country. Physicians and students living in restricted states are scared for the health of their patients, as well as their own healthcare. They feel trapped by the state legislature brought by the Dobbs decision and worry about the consequences that have already been experienced, as well as future implications.
